Covid-19 and Insecure Work
Our analysis shows that the statutory sick pay system is failing insecure workers.
Insecure workers are nearly 10 times more likely to say they receive no sick pay compared to secure workers.
The shocking disparity in sick pay between workers in secure and insecure employment was revealed by recent TUC polling carried out by Britain Thinks.
67% of insecure workers say they receive nothing when off sick compared with 7% of secure workers who reported receiving nothing when off sick.
It provides a stark example of how inadequate employment protections compel insecure workers to continue working throughout the pandemic. Insecure workers who need to self-isolate or take time off sick, have to continue going to work in order to pay the bills.
Recommendations and action plan
The TUC believes that three key actions need to take place:
Increasing and enhancing sick pay entitlement
The government should:
- abolish the earnings threshold for statutory sick pay, extending coverage to almost two million workers
- for all absences, remove the waiting period for sick pay
- increase sick pay to £330 a week, the equivalent of a week’s pay at the real living wage
- provide additional funds to ensure employers can afford to pay sick pay.
New rights for workers to benefit from the protection that collective bargaining brings
We are calling for:
- unions to have access to workplaces to tell workers about the benefits of union membership and collective bargaining.
- new rights to make it easier for working people to negotiate collectively with their employer.
- the establishment of new bodies for unions and employers to negotiate across sectors, starting with hospitality and social care.
A ban on zero-hours contracts
We are calling for:
- the effective abolition of zero hours contracts by giving workers the right to a contract that reflects their regular hours
- at least four weeks’ notice of shifts, and
- compensation for cancelled shifts.
Download full report (pdf)
Executive Summary
We rely on key workers to get us through the pandemic. Care workers and nurses care for our friends and family members when they are taken ill. Delivery drivers make sure we have food and other essential items delivered to our homes.
Many of these workers are on insecure contracts, such as zero-hours contract workers or agency workers. Insecure work is often done by people who already face disadvantage and discrimination, with women, disabled workers and those in minority ethnic groups more likely to be working in insecure jobs. 1
Insecure workers lose out on pay and employment rights – they have no safety net
Insecure workers face job and income insecurity. Week to week, they don’t know whether they will have work or money coming in. An agency worker may find that their work dries up if their recruitment agency can’t find them an assignment. A zero-hours contract worker may not be given any shifts by their employer.
These workers face increased precarity during the pandemic. Insecure work already carries a pay penalty, so insecure workers face increased financial insecurity through a double whammy of low pay and increased unemployment resulting from the pandemic.
Insecure workers are unlikely to benefit from the full range of employment rights that permanent, more secure workers are entitled to. These include vital safeguards such as unfair dismissal and redundancy protections.
Recently introduced government support mechanisms are inadequate to protect insecure workers
Government support mechanisms such as the Coronavirus Job Retention Scheme, Universal Credit and other self-isolation funds provided an inadequate financial safety net for insecure workers. While some have secured vital support, others have faced hardship or felt forced to carry on working even when it is unsafe for them to do so.
The nature of insecure work is a contributory factor to the scale and severity of the Covid-19 pandemic
This report explores how the nature of insecure work has exacerbated the scale and severity of the pandemic. We look at the following issues:
- Insecure workers are nearly ten times more likely than secure workers not to receive any sick pay.
- Insecure workers are subject to exploitative working conditions such as dirty working environments and often share cramped accommodation.
- The transient and peripatetic nature of insecure work brings insecure workers into contact with more people.
- Health and safety safeguards are less rigorously implemented for insecure workers.
Insecure, key workers who were at the forefront of the fight against Covid-19 are now being overlooked during the recovery.
Our report identifies the key reforms that are needed to eradicate insecure work and build back better after the pandemic.
The pandemic should be a catalyst for change. Everyone deserves decent work.
What is insecure work?
There are 3.7 million people who face insecurity in work in the UK, either because their contract does not guarantee regular hours or income (including zero-hours contracts, agency work and casual work) or because they are in low-paid self-employment (earning less than the government’s National Living Wage). In total, this is one in nine in of those in work.
Insecure work isn’t just found among the food delivery riders and taxi-drivers of the new app-based platform economy, who are prominent in discussion of the topic. Though it is rife in these roles, many of those in insecure work are in the sorts of key workers – carers, delivery drivers, shopworkers – whose worth to society was brought sharply to attention during the pandemic. 2
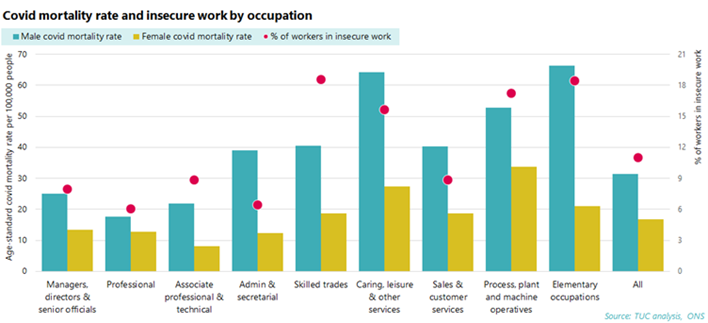
For example, nearly one in six (15.6 per cent) of those in caring, leisure and other service roles were in insecure work, according to our analysis of official figures. Nearly one in five (18.4 per cent) of those in elementary roles, such as security guards, taxi drivers and shop assistants, and a similar number of those in skilled trades (18.5 per cent) are in insecure work as are 17.2 per cent of process, plant and machine operatives. This compares to 6 per cent of those in professional roles and 6.4 per cent of those in administrative or secretarial jobs.
Who does insecure work? Which people are most affected?
Insecure work is often done by people who face disadvantage and discrimination, with women, disabled workers and those in minority ethnic groups more likely to be working in insecure jobs.
Disabled workers
Our evidence shows disabled workers are more likely to be employed in some kind of insecure work. 3
TUC analysis found that disabled workers are more likely to be employed on zero-hours contracts (ZHCs). While 3.1 per cent of non-disabled workers are employed on a ZHC, this rises to 3.8 per cent of disabled workers.
Women
Women are more likely to be in insecure work (excluding self-employment) - with 7.1 per cent of women in this type of insecure work compared to 6 per cent of men 4
.
BME workers and insecure work
BME workers have been asked to shoulder more risk during the pandemic, often working in insecure jobs with fewer rights at work. 5
.
TUC analysis shows that BME people are far more likely to be in precarious work and in jobs with higher coronavirus mortality rates than white people, such as security guards, carers, nurses and drivers. Our analysis shows that 1 in 6 (16%) BME workers are employed on insecure terms and conditions, compared to 1 in 10 (10%) white workers.
BME staff are at higher risk of Covid-19 exposure and job loss. Insecure contracts make it more difficult for workers to:
- assert their rights for a safe workplace with adequate protective equipment (PPE)
- shield if they – or someone they live with – has a health condition that puts them at higher risk
- take time off for childcare responsibilities if schools or childcare providers close.
Black and minority ethnic (BME) women
BME women face even more precarity. BME women are around twice as likely as white workers to be employed in insecure jobs, according to TUC analysis. 6
.
The analysis shows that around 1 in 8 (12.1 per cent) BME women working in the UK are employed in insecure jobs compared to 1 in 16 (6.4%) white women and 1 in 17 (5.5%) white men.
Lack of workplace rights, and the knowledge that hours can be reduced or temporary contracts not renewed, shapes the workplace experience of BME women in insecure work. The stress and uncertainty created by the unpredictable nature of insecure work blights the lives of workers in ordinary times. But the Covid-19 pandemic has added a more deadly aspect to this lack of workplace power and protection. BME workers have told the TUC they are frequently denied access to Personal Protective Equipment (“PPE”) and to appropriate risk assessments.
Why does insecure work exacerbate problems in the pandemic?
Inadequate sick pay and insecure work
Many insecure workers miss out on sick pay altogether or are forced to rely on Statutory Sick Pay (SSP).
Current problems with the sick pay system
The lack of decent sick pay is a barrier to self-isolation. Recent ONS figures 7
show that 13 per cent of people receive no pay or sick pay at all while self-isolating, and there is widespread evidence, including from Baroness Harding 8
. While we welcomed the additional funding announced in February, this remains a complex and inadequate system.
The likelihood of the coronavirus pandemic remaining with us for some time means it is vital that we have a decent sick pay system in place. People need to be confident that they can take time off work when they have are ill, and this will be key to the success of any workplace testing or certification scheme.
Low level of SSP makes it an unaffordable option for many insecure workers
Those who do receive SSP may struggle - at £96.35 the average worker would lose around 80 per cent of their earnings. This rate is extremely low internationally – on average, OECD countries provide support worth around 70 per cent of earnings 10
. Previous TUC research shows over 4-in-10 workers (43 per cent) told us that they would have to go into debt or not pay bills if their income dropped down to £96 per week for two weeks. 11
Insecure workers already experience a pay penalty when compared to the pay of an average employee. 12
For these workers, money may already be tight, with fewer savings in the bank to fall back on. Self-isolation or taking time off sick may not be a realistic option for insecure workers with financial commitments.
The lack of adequate sick pay system forces people to make an impossible choice between isolating and paying their bills.
Eligibility criteria excludes many insecure workers from accessing SSP
To be eligible for SSP, an employee must, on average, earn £120 per week. This excludes 1.8 million employees, 70 per cent of whom are women. This particularly impacts young workers, older workers, those on zero-hours contracts, and low-paid occupations.
Around a third of those on zero-hours contracts do not qualify for sick pay, compared to 6 per cent of permanent employees. This is because their irregular hours may not result in them earning enough to meet the income threshold. 13
The income threshold eligibility criteria means that those in insecure jobs may force themselves in to work even if they are unwell – putting their clients’ or fellow workers’ health at risk.14
Job insecurity means workers fear losing their jobs if they call in sick
Insecure workers have told us that they are reluctant to take sick leave because they fear that their employer will find someone else to do their jobs if they don’t turn up. Job insecurity is a key element of insecure work. Many of those in insecure work can be fired without notice. For example, an employer can call a recruitment agency and ask them not to send the agency worker back into work. For those on zero hours contracts, they have no guaranteed hours, so the employer is not obliged to offer them work.
Government inaction
The inadequacies of SSP mean that many insecure workers do not have a safety net to rely on, if they become ill. A situation which was brutally exposed during the pandemic when many workers felt compelled to carry on working rather than self isolating. Unions campaigned for an increase to sick pay before the severity of pandemic intensified as we could see the inevitable consequences of an inadequate sick pay support system.
The government failed to act. The situation was avoidable.
At the beginning of the pandemic Matt Hancock, the Health Secretary, confirmed that he wouldn’t be able to afford to live on Statutory Sick Pay. 15
Instead of raising sick pay, in September, more than six months into the pandemic, the government introduced a £500 payment for those on low incomes who have been told to self-isolate by NHS Test and Trace. But TUC research has shown that it has failed to meet demand for support. Our findings shows that the scheme is failing to financially support workers who have been required to self-isolate. This is for two reasons: the eligibility criteria for the main payment means that many workers miss out; and the lack of funding for the discretionary scheme means most applicants are rejected.
In March 2021, Matt Hancock was allegedly pushing for an increase in sick pay. 16
Despite recognising that sick pay is inadequate, a year of government inaction has undoubtedly worsened the impact of the pandemic.
Lack of sick pay for agency care staff leads to higher COVID infection levels.
An Office for National Statistics study 17
confirmed that insecure work is a contributory factor to higher Covid-19 infection levels. The study showed that care homes in England that use more agency staff or do not offer sick pay are more likely to have higher levels of Covid-19 infection among residents. Care homes using bank or agency nurses or carers most days or every day are more likely to have more cases in residents compared with those care homes who never use bank or agency staff. And care homes in which staff receive sick pay are less likely to have cases of coronavirus in residents, compared with those care homes where staff do not receive sick pay. |
Poor working conditions and exploitation of insecure workers
Unions have revealed that poor working conditions and exploitative working practices associated with agency work, have worsened during the pandemic.
Unite the Union has raised the alarm on the link between migrant worker exploitation and Covid-19 outbreaks in the meat processing sector.18
Unite said there is also a direct correlation between the treatment of migrant staff as “disposable assets” and the spread of the disease in such environments. There are a number of reasons for this:
- Meat processing factories are less likely to provide agency staff that need to self-isolate with company sick pay or any other form of financial support, which increases the danger of individuals with Covid-19 going into work because they cannot afford to take time off.
- There are concerns that track and trace record keeping for agency workers is not being carried out properly. For example, production line staff and cleaners, who often work at multiple sites and whose contact details may not be available, could be overlooked during infection control procedures.
- Agency staff working in the meat processing sector are often placed in overcrowded housing which are a contributing factor to the risk of outbreaks within factories. A Unite survey, comprising 20 per cent of the workforce at a Covid-19 impacted meat processing plant staffed overwhelmingly by migrant workers, found that:
- 43 per cent of respondents live with two or more colleagues (at least three to a house) and 11 per cent live with five or more.
- Nearly 65 per cent of the 150 respondents said they have attended work whilst unwell, with 69 per cent of those doing so because they could not afford to lose pay.
Unite the Union showed that the dire working conditions in the meat processing sector including low pay and insecure employment have hindered the nation’s efforts to defeat the coronavirus.
Transient and peripatetic nature of insecure work
The nature of insecure work means that many insecure workers such as agency workers or zero hours contract workers might work on:
- assignments or contracts for short periods meaning they change jobs and workplaces, frequently coming into contact with a wider range of people than those who work at permanent, fixed locations and/or
- as part of their normal work (such as care workers) travel between work locations on a frequent basis, coming into contact with a wider range of people than those who work at permanent, fixed locations
An unpublished Public Health England study 19
, shared with care home providers, confirmed the increased level of risk associated with insecure work and higher levels of COVID infections and death rates. The study, which used genome tracking to investigate outbreaks, found that temporary care workers transmitted Covid-19 between care homes as cases surged. The report showed that agency workers – often employed on zero-hours contracts – unwittingly spread the infection as the pandemic grew.
The genome tracking research into the behaviour of the virus in six care homes in London found that, in some cases, workers who transmitted coronavirus had been drafted in to cover for care home staff who were self-isolating expressly to prevent the vulnerable people they look after from becoming infected.
The study warned that “Infection is spreading from care home to care home, linked to changed patterns of staffing, working across and moving between homes.” The infection could be introduced by “bank staff” – floating workers used to fill temporary vacancies in different homes – it said, adding that workers were often asymptomatic so “by the time local health protection teams are informed of an outbreak substantial transmission may already have occurred”.
A study 20
by the medical journal, The Lancet, also confirmed that “compared with no employment of agency nurses or carers, frequent (ie, on most days or every day) employment of agency nurses or carers was associated with a significantly increased odds of infection in residents.”
This situation was avoidable. A 2019 Public Health England (PHE) document about flu pandemic preparations called “Infection prevention and control: an outbreak information pack for care homes” urged operators to “try to avoid moving staff between homes and floors”. Despite this knowledge, safeguards were not considered and implemented until May 2020, which meant that infection and death levels increased unnecessarily in care homes during that period.
Lack of proper PPE for insecure workers
Throughout the pandemic, workers in insecure employment have reported not having access to adequate, sufficient personal protective equipment that would protect both themselves and the members of public that they come into contact with.
The Fairwork Foundation, highlighted that whilst 60 percent of the platforms claimed to provide PPE (disinfectant or, less often, masks) workers often reported problems receiving any of that support.21
Similarly, the Royal College of Nursing has provided evidence that agency nurses have received inadequate levels of PPE compared with their permanent counterparts.22
This lack of PPE means that insecure workers and the people they come into contact with have an increased risk of catching COVID.
| In April 2020, Nomusa and agency nurse contracted the virus herself and was ill for a month. “I know exactly where I got it from,” she says. “I’d been told that a care home had full PPE but when I got there it was literally a plastic apron and a mask. At this point, those working in hospitals were wearing full PPE, with visors and everything else. It was inevitable it would happen.” |
Insecure workers already in a more precarious financial position
Insecure workers face a pay penalty
Insecurity and low pay go hand-in-hand.
TUC analysis 23
shows that all categories of insecure worker is paid significantly less than employees in general. So not only are many insecure workers vulnerable to the sudden withdrawal of work, but they also have less capacity to withstand shocks to their income because their wages do not allow them to build a savings buffer.
Our analysis shows the median gross hourly pay for those in casual work amounted to £8.03 an hour in 2019, for seasonal work £8.10 and for zero hours workers £8.17. Those working for an employment agency typically received £9.69. But this is well behind the £12.25 average for all employees.
This is significant as it shows that lower paid, insecure workers are more likely to face financial insecurity during the pandemic, especially if they need to take time off sick or to self-isolate.
Insecure workers have faced a cut in income and been forced to make savings during the pandemic
TUC research 24
has also shown that:
- 55 per cent of those in insecure work have experienced a cut in their income.
- 44 per cent of those in insecure work have had to cut back, compared to a third of those in secure work
Both of these factors indicate that financial insecurity could be a key driver for insecure workers to continue working when sick or self-isolation leave should be taken.
Government support funds for specific sectors are not fit for purpose
The government launched an infection control fund designed to ensure care staff were “not penalised” for staying away from work.
The scheme was supposed to ensure staff are fully compensated if they need to stay off work because they tested positive for Covid-19, were showing symptoms or were shielding.
But a UNISON survey 25
of care workers revealed the money did not get through to workers, with more than two fifths (44%) saying their employer is offering just statutory sick pay (SSP) of £95.85. Around one in 12 (8%) workers say they and colleagues were not paid at all if they needed to stay at home.
This poorly designed scheme failed to funnel money to the workers who needed financial support when self-isolating. UNISON showed that over half of care workers had to rely on the paltry statutory minimum sick pay. As we’ve shown above, the inadequacy of SSP meant that workers were compelled to carry on going to work so they could pay their bills.
Insecure workers and the furlough scheme
The government’s wage support schemes introduced during the pandemic had a patchy impact on insecure workers.
While many have had vital support, some have missed out on any support while others have seen their incomes drop below the minimum wage.
Since March 2020, the Coronavirus Job Retention Scheme (CJRS) has supported the wages of 11.2 million people and the Self-Employment Income Support Scheme (SEISS) has helped around 2.7 million self-employed people.
Importantly, the rules for the CJRS allowed employers to place zero-hours and agency worker on furlough.
But, crucially, there was no obligation for them to do so, so many simply stopped offering shifts. The same fate befell some casual freelancers in sectors like journalism.
A large number of workers also fell between the scheme designed for self-employed workers and the furlough scheme for employees.
To qualify for the self-employed scheme a worker needed to have obtained more than half their income from such work.
Many of those, notably in sectors like arts and theatre, fell foul of this rule because they combined employed work, for example in schools, with freelance work.
In all, some three million workers are estimated to have missed out on support for various reasons.26
Another notable flaw in the wage support schemes is that they have not stopped workers’ wages falling below the level of the minimum wage.
ONS survey data from October 2020 shows that around four-in-10 furloughed employees in the private sector didn’t receive a top up to their wages, beyond the 80 per cent they were required to receive.
The Annual Survey of Hours and Earnings (ASHE), conducted in April 2020, found that low-paid workers were the most likely not to have their pay topped up.
As a result, two million people were being paid below the minimum wage in April 2020, with around 1.3 million of these being furloughed employees on reduced pay. 27
Another notable flaw in the wage support schemes is that they have
This reflects the fact that more than half of employees in the lowest decile of hourly earnings were furloughed and receiving reduced pay.
The proportion of employees furloughed without being paid the top-up was highest in industries such as hospitality (39 per cent), the arts (27 per cent), and construction (26 per cent). 28
Social security networks failing insecure workers – Universal Credit
Insecure workers get a tougher deal in Universal Credit. During the pandemic, Universal Credit is a vital safeguard for many workers facing unemployment through redundancy or illness, many insecure workers wouldn’t be entitled to redundancy pay or unfair dismissal protections, so would have found themselves unemployed without notice or compensation. And there is a minimum of a five week wait for the first payment.
Five-week wait for payment
Under the design of Universal Credit, claimants must wait five weeks for their first payment. This means at the point when people are most vulnerable, the system fails to support them and adds to the turbulence of their finances. There is no justification for the five-week wait for a first payment of Social Security.
Monthly assessment period
Those in insecure work face a further challenge in Universal Credit as the design of the monthly assessment periods do not work well for them. This group of workers are more likely to experience fluctuations in their income due to irregular hours, but the design of Universal Credit is better suited to those with stable hours and income.
Insecure work is convenient for employers. Quick to hire and easy to fire
During the economic downturn triggered by the pandemic, insecure workers have been disproportionately affected by job losses. Firms are sheltering permanent workers more than those on temporary contracts. The workers who are employed to carry out vital service such as caring, deliveries and Covid-19 testing are being employed on insecure contracts.
Insecure workers and job losses in the pandemic
In a recession, workers in insecure employment will typically be first to lose their jobs. It’s more convenient for an employer to terminate the employment of an insecure worker, as they are unlikely to be entitled to redundancy or unfair dismissal protections.
A report 29
by the IZA Institute of Labour Economics confirms that the impact of this recession on insecure workers, follows previous trends. They found the following:
- The outbreak has caused significant disruptions to the economy but the impact has been unequal across different types of jobs. Employees in permanent contracts and in salaried jobs were significantly less likely to lose their jobs compared to employees in other alternative work arrangements.
- Employees in less secure work arrangements are more likely to have lost their jobs following the coronavirus outbreak. In the UK, employees with a permanent contract are 17 percentage points less likely to have lost their job relative to employees on temporary contracts.
- Firms are sheltering permanent workers more than those on temporary contracts. Even amongst those on permanent contracts, workers on flexible hours contracts or who are paid by the hour have been hit hardest.
Insecure workers are being employed to carry out vital Covid-19 services
Private Eye 30
has reported that staff at NHS Covid-19 testing sites run by G4S, are not actually employed by G4S.
Covid-19 testing sites help to stop the spread of the virus. They make sure people can get tested, and where necessary, self-isolate promptly. The people carrying out this vital work should be rewarded with decent, secure employment. Instead, the government has awarded the contract to G4S who, by using a range of labour market intermediaries, have shirked their responsibilities to the people who do work for them at the Covid-19 testing sites.
Private Eye reports that G4S was paid £57m to operate the Covid-19 testing sites for the first six months they have been in operation.
G4S uses a recruitment agency, “HR GO”, to source the workers. “HR GO” appears to use an umbrella company to operate their payroll. Private Eye suggests that this umbrella company has setup a number of “mini umbrella”31
, additional labour market intermediaries, who are the legal employers of these workers.
The TUC believes funnelling money to umbrella companies in this way is a misuse of public money. The key workers operating these Covid-19 test sites should be respected and offered decent working conditions. Instead G4S has chosen to use a recruitment agency which has deliberately extended its supply chain by using labour market intermediaries for “commercial reasons”, with little regard for the impact this has on the key workers at the Covid-19 testing sites.
The use of umbrella companies distorts the employment relationship. Workers using umbrella companies have reported not being sure who their employer is and who to speak to when problems arise.
Insecure workers are at the forefront of the fight against Covid-19 – but they are being overlooked in the recovery
There is evidence that insecure workers found themselves at the back of the vaccination queue and treated less favourably than their permanent counterparts.
This is a common feature of a two-tier workforce – insecure workers can be treated as an afterthought, as employers focus on their core, permanent workforce.
The Royal College of Nursing has recognised the success of the vaccine rollout across England 32
, but has warned that agency and temporary nursing staff at risk of being left behind.
The RCN reported 33 , in February 2021, that more than two in five agency nursing staff and one in four temporary staff, who often cover short-staffed areas, had not received a vaccine – compared to just one in eight hospital workers.
There is a correlation between insecure work occupations and higher COVID death rates
Our analysis shows that Covid-19 mortality rates are highest in the top four sectors that are synonymous with insecure work.
We’re concerned that Covid-19 mortality rates in insecure jobs twice as high as other occupations during the pandemic. The analysis shows that:
- The Covid-19 male mortality rate in insecure occupations was 51 per 100,000 people aged 20-64, compared to 24 per 100,000 people in less insecure occupations.
- The Covid-19 female mortality rate in insecure occupations was 25 per 100,000 people, compared to 13 per 100,000 in less insecure occupations.
We know that the reasons for mortality rates during the coronavirus pandemic are complex. But it is notable that in an analysis of mortality rates by occupation, rates were significantly higher in occupations also characterised by insecure work. Further research is needed to understand the links, which could include the fact that many of these occupations include work outside the home and that many insecure workers lack decent sick pay.
Recommendations and action plan
The pandemic has exposed the lack of dignity that many insecure workers face. Society relies on these workers to carry out vital roles such as caring for sick people and delivering vital food and other services. In return, a significant number of these workers will have no job or income security.
This needs to change. A first step would be to ban exploitative zero hours contracts and provide people with guaranteed hours contracts.
The pandemic has exposed the detrimental impact of insecure work both for the workers employed on these contracts and wider society.
The TUC believes that three key actions need to take place:
Increasing and enhancing sick pay entitlement
It’s vital that sick pay is reformed, to give workers who are ill or those who need to self-isolate, a proper financial safety net that enables them to meet their financial commitments whilst they are off work.
The government should:
- abolish the earnings threshold for statutory sick pay, extending coverage to almost two million workers
- for all absences, remove the waiting period for sick pay
- increase sick pay to £330 a week, the equivalent of a week’s pay at the real living wage
- provide additional funds to ensure employers can afford to pay sick pay.
For further details on our policy recommendations relating to decent sick pay for all please see the TUC report, A Safe Return to the Workplace
New rights for workers to benefit from the protection that collective bargaining brings
Trade unions can help insecure workers negotiate secure employment. Workers and unions need additional rights to make it easier for unions to raise employment standards.
We are calling for:
- unions to have access to workplaces to tell workers about the benefits of union membership and collective bargaining.
- new rights to make it easier for working people to negotiate collectively with their employer.
- the establishment of new bodies for unions and employers to negotiate across sectors, starting with hospitality and social care.
For further details on our policy recommendations relating to collective bargaining please see details of our campaign, A stronger voice for workers.
A ban on zero-hours contracts
As a priority, we need to raise minimum standards and provide workers with much needed security.
We are calling for:
- the effective abolition of zero hours contracts by giving workers the right to a contract that reflects their regular hours
- at least four weeks’ notice of shifts, and
- compensation for cancelled shifts.
For further details on our policy recommendations for insecure workers please see the TUC report, Insecure work, Why decent work needs to be at the heart of the UK’s recovery from coronavirus.
- 1 (2020). “BME women are twice as likely to be in insecure jobs as white workers”, TUC.
- 2 (2020).”Insecure work: Why decent work needs to be at the heart of the UK’s recovery from coronavirus”, TUC.
- 3 (2020). “Disability pay and employment gaps”, TUC.
- 4 Sharp, T. (2020). “With 3.6 million in insecure work, we have an opportunity for change”, TUC
- 5 (2020), “BME workers have been asked to “shoulder more risk” during pandemic, says TUC”, TUC.
- 6 (2020), “BME women and work”, TUC.
- 7 Fok, A. (2021). “Coronavirus and self-isolation after testing positive in England: 1 February to 13 February 2021”, Office for National Statistics.
- 8 Tolhurst, A. (2021). “Dido Harding Admits 20,000 People A Day Are Ignoring Calls By NHS Test And Trace To Self-Isolate”, PoliticsHome [/fn}, that financial barriers are one of the reasons for non-compliance with an instruction to self-isolate. The fact that almost two million workers do not qualify for SSP due to the lower earnings limit is clearly a major issue when it comes to requiring low earners to self-isolate.
The self-isolation payment is not an adequate substitute for decent sick pay. We found that seven in ten workers were being refused payment
(2021). “Sick pay that works”, TUC. - 10 Reed, S & Palmer, B. (2021). “To solitude: Learning from other countries on how to improve compliance with self-isolation”, Nuffield Trust.
- 11 Collinson, A. (2020). “Why we need an increase in statutory sick pay”, TUC.
- 12 Ibid. 2
- 13 Ibid. 9
- 14 Ibid. 9
- 15 Cockburn, H. (2020). “Coronavirus: Matt Hancock admits he couldn't live on statutory sick pay”, The Independent.
- 16 Cowburn, A. (2021). “Matt Hancock pressing for ‘increase in statutory sick pay’”, The Independent.
- 17 Tinsley, B. (2020). “Impact of coronavirus in care homes in England: 26 May to 19 June 2020”, Office for National Statistics.
- 18 (2020). “Link between migrant worker exploitation and Covid-19 meat processing outbreaks ‘must be addressed’”, Unite the Union.
- 19 Booth, R. (2020). “Agency staff were spreading Covid-19 between care homes, PHE found in April”, The Guardian.
- 20 Multiple authors. (2021). “Factors associated with SARS-CoV-2 infection and outbreaks in long-term care facilities in England: a national cross-sectional survey”, The Lancet.
- 21 (2020). “The Gig Economy and Covid-19”, The Fairwork Foundation.
- 22 (2020). “Inside care homes: the agency perspective”, RCN bulletin.
- 23 Ibid. 2
- 24 (2021). “The impact of the pandemic on household finances”, TUC.
- 25 (2020). “Care staff aren’t getting proper sick pay promised by ministers, UNISON survey shows”, UNISON.
- 26 (2020). “How effective are the coronavirus safety nets?”, Standard Life Foundation.
- 27 Smith, R. (2020). “Jobs paid below minimum wage by category”, Office for National Statistics.
- 28 Collinson, A. (2020). “The government must ensure no one is paid below the minimum wage due to the furlough scheme”, TUC.
- 29 Adams-Prassl, Abi et al. (2020). “Inequality in the Impact of the Coronavirus Shock: Evidence from Real Time Surveys”, I Z A Institute of Labour Economics.
- 30 Hughes, S. (2021). “Pay Slippery”, Private Eye.
- 31 For a further explanation of “mini umbrellas” please see this TUC commissioned report: (2021). “Labour Market Intermediaries”, Chartered Institute of Taxation.
- 32 (2021). “Temporary nursing staff at risk of being left behind on vaccines”, Health Business.
- 33 (2021). “Vaccine rollout a success so far but RCN warns agency and temporary nursing staff at risk of being left behind, Royal College of Nursing
Stay Updated
Want to hear about our latest news and blogs?
Sign up now to get it straight to your inbox